Vol 4 | Issue 1 | Jan-Apr 2018 | page: 19-20 | Chitta R Mohanty, Satyabrata Guru, Upendra Hansda, Sadananda Barik
Authors: Chitta R Mohanty [1], Satyabrata Guru [1], Upendra Hansda [1], Sadananda Barik [1]
[1] Department of Trauma and Emergency Medicine,All India Institute of Medical Science, Bhubaneswar. India.
Address of Correspondence
Dr. Chitta R Mohanty,
Department of Trauma and Emergency Medicine, All India Institute of Medical Science, Bhubaneswar. India.
E-mail: tem_chitta@aiimsbhubaneswar.edu.in
Abstract
Introduction: Complete heart block is a rare disorder of conduction system which can be congenital oracquired.Anesthesia in patients with complete heart block can be challenging to anesthetist.
Case Report: We report a 25-year-old female presented for emergency cesarean section with fetal distress found to have complete heart block. We discuss the management of patient with complete block posted for surgery according to advanced cardiac support guidelines with review of literature.
Conclusion: Anesthesia in patients with complete heart block can be challenging due to uncontrolled hemodynamics unresponsive to conventional drugs. Anesthetic management in such patients should be according advanced cardiac life support guidelines. General anesthesia is preferred over spinal anesthesia for better control of hemodynamics.
Keywords: Transcutaneous pacemaker, complete heart block, emergency cesarean section.
Introduction
A 25-year-old female with 36 weeks pregnancy (gravida 2 para1) with a history of previous cesarean section presented with fetal distress for emergency cesarean section. Previous cesarean section was uneventful. The patient was found to having the third-degree heart block and rate of 52 beats per minute. As per literature, this rare presentation during pregnancy was reported, but in all other instances, the patient had time to insert a temporary transvenous pacemaker. We present the first case wherein the patient presented with fetal distress for emergency cesarean section where transcutaneous pacemaker was only optioned with cardiac drugs according to advanced cardiac support guidelines for patient management.
Case Report
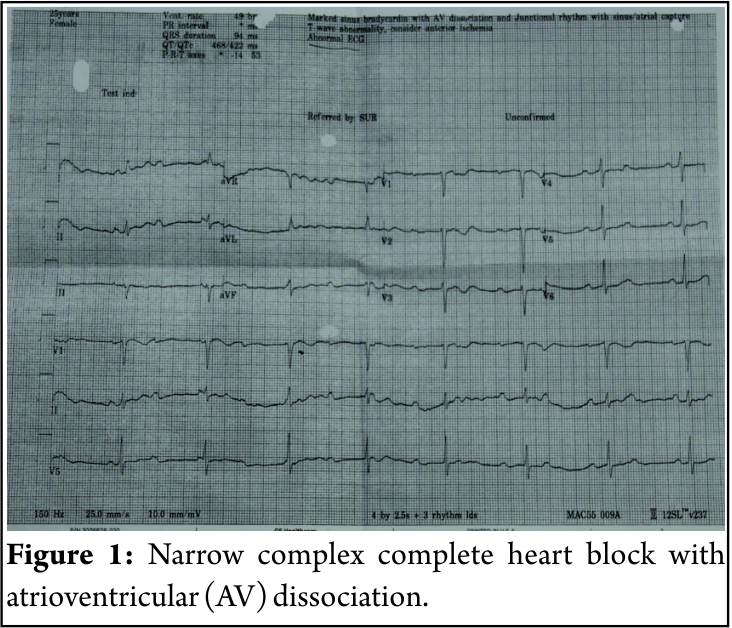
A 25-year-old female with a history of previous cesarean section was presented for emergency cesarean section due to fetal distress. Previous cesarean section under spinal anesthesia 2 years back was uneventful. Only investigation was hemoglobin 11.2mg%. In the pre-operative room,the patient had pulse rate of 52 beats per minute, SPO2 99%, and blood pressure (BP) -124/68 mmHg. There was narrow complex the third-degree heart block on electrocardiograph monitor.Heart rate remained unchanged with intravenous 1.2 mg atropine. High-risk consent was explained and taken from the patient. The patient had fetal distress, and there was not enough time to implant a transvenous temporary pacemaker. Hence, transcutaneous pacemaker, emergency cardiac drugs epinephrine infusion was kept ready as per advanced cardiac support guidelines.The left radial arterial cannula was inserted before induction to monitor pulse rate and precise BP monitoring. Baseline arterial blood gas was sent. Rapid sequence induction was done with injection thiopentone 250mg, injection fentanyl 1 microgram per kg,and succinylcholine 1mg/kg intravenously and intubated with 7.0 mm endotracheal tube. Anesthesia was maintained with nitrous oxide and oxygen at 1:1 ratio with 0.6% isoflurane. One episode of hypotension with SBP <90 mmHg was treated with 6 mg ephedrine IV which raised heart rate to 68 beats per minute. A healthy male child was delivered with Apgar score 8 at 1 min and 9 at 5 min. At the end of surgery, neuromuscular blockade was reversed with combination of neostigmine 2.5 mg and glycopyrrolate 0.5 mg.Post-operative period was uneventful.The next day 12 lead electrocardiogram (ECG) along with ECHO was done. In ECG, there was narrow complex complete heart block with atrioventricular (AV) dissociation (Fig. 1). In ECHO, there was moderate mitral regurgitation, good left ventricular function, and bradycardia noted during study.The patient gavea history on and off dizziness. A diagnosis of congenital complete heart block was made. The patient was advised for the insertion of permanent pacemaker.
Discussion
Complete heart block is a rare disorder of conduction system which can be congenital or acquired. Congenital heart block may occur as isolated or in association with other cardiac abnormalities. Complete heart block is most commonly seen in older patients having chronic degenerative changes in their conduction system. Digitalis intoxication may also lead to complete heart block. Complete heart block may occur abruptly after open heart surgery,particularly after aortic valve replacement and as complication of acute anterior myocardial infarction. The first- and second-degree heart blocks are examples of incomplete block because the AV junction conducts at least some stimuli to ventricles. With complete heart block, no stimuli are transmitted to atria from ventricles.Instead the atria and ventricles are paced independently. With complete heart block, the QRS complex may be either of normal width or abnormally wide with appearance of a bundle branch block pattern. As a general rule, complete heartblock with wide QRS complexes tends to be less stable than complete heart block with narrow QRS complex because escape pacemaker is usually slower and less consistent [1]. Noninvasive transcutaneous pacing is a technique of electrically stimulating the heart externally through a set of electrode pads. The stimulus is intended to cause cardiac depolarization and myocardial contraction. Pacing is one method of treating patients when their heart’s own conduction system slows dangerously. Indication of emergency pacing includes Class I – hemodynamically symptomatic compromising bradycardia that is too slow and unresponsive to atropine. Symptoms include BP<80 mmHg systolic, changes in mental status, angina, and pulmonary edema. Class IIa –bradycardia with escape rhythms unresponsive to pharmacologic therapy, symptomatic sinus nodedysfunction, Mobitz II second-degree heart block. Class IIb override pacing of either supraventricular or ventricular tachycardia that is refractory to pharmacologic therapy or electrical cardioversion [2]. Non-invasive transcutaneous pacemakers operate in fixed rate mode and demand rate mode. In fixed rate mode, the pace rate is set by clinician regardless of patient’s intrinsic heart rate. In demand mode pacing, the pacer senses the patient’s intrinsic heart rate and will pace if intrinsic signal is slower than the rate programmed by the clinician[3]. In symptomatic pregnant patients,permanent pacemaker should be implanted in the first trimester.The patient undergoing elective surgery prophylactic temporary transvenous pacemaker can be implanted before surgery [4,5]. In our case, the patient was presented in emergency with fetal distress and there was not adequate time to insert a temporary transvenous pacemaker, so transcutaneous pacemaker with cardiac drugs according to advanced support guidelines was the only option [6].
Anesthetic challenges in complete heart block can be bradycardia and hypotension unresponsive to conventional drugs, cardiac arrest, or sudden cardiac death. With spinal anesthesia in pregnancy, there can be rapid hemodynamic imbalance and hypotension and bradycardia, as well as difficulty to control the level of block. Jordi et al. have reported the third-degree heart block and asystole associated with spinal anesthesia [7]. General anesthesia with invasive arterial BP monitoring for precise control of heart rate and BP along with cardio selective anesthetic agents is the safer option.
Conclusion
Anesthesia in patients with complete heart block can be challenging due to uncontrolled bradycardia and hypotension unresponsive to conventional drugs. For elective surgery, permanent or temporary pacemaker insertion should be inserted before surgery. For emergency surgery,temporary transcutaneous pacemaker along with emergency cardiac drugs should be kept ready. General anesthesia is preferred over spinal anesthesia for better control of hemodynamics.
References
1. Goldberger AL. Clinical Electrocardiography a Simplified Approach. 7th ed. Philadelphia, PA: Elsevier; 2006. p. 203-10.
2. Bartecchi CE. Temporary cardiac pacing—diagnostic and therapeutic indications. Postgrad Med 1987;81:269-77.
3. Béland MJ, Hesslein PS, Finlay CD, Faerron-Angel JE, Williams WG, Rowe RD, et al. Noninvasive transcutaneous cardiac pacing in children. Pacing ClinElectrophysiol1987;10:1262-70.
4. Mehta S, Goswami D, Tempe A. Successful pregnancy outcome in a patient with complete heart block. J Postgrad Med 2003;49:98.
5. Mohan VK, Naik AK, Bharti N, Shende D. A patient with congenital complete heart block undergoing multiple exposures to general anaesthesia. Anaesth Intensive Care 2003;31:667-71.
6. Michel W, Kenneth N, Katherine B, Soderberg ES, Callaway SW. Advanced Cardiovascular Life Support Provider Manual. Texas: American Heart Association; 2016. p. 120-8.
7. Jordi EM, Marsch SC, Strebel S. Third degree heart block and asystole associated with spinal anesthesia. Anesthesiology 1998;89:257-60.
| How to Cite this Article: Mohanty C R, Guru S, Hansda U, Barik S. Anesthetic management of a patient with congenital complete heart block posted for emergency cesarean section. Journal of Anaesthesia and Critical Care Case Reports Jan-Apr 2018; 4(1): 19-20 |