Vol 5 | Issue 2 | May-Aug 2019 | page: 13-15 | Deepali Gomase Rahate
Authors: Deepali Gomase Rahate [1]
[1] Department of Anaesthesia, Ganga Care Hospital, Nagpur, Maharashtra
Address of Correspondence
Dr. Deepali Gomase Rahate,
Department of Anaesthesia, Sr. Consultant,
Ganga Care Hospital, Nagpur, Maharashtra.
Email:drdeepaligomase@gmail.com
Abstract
We reported a 51 days baby who was admitted with complaints of increased gastroesophageal reflux with repeated aspiration pneumonia and requiring ventilator support off and on. Patient was posted for bronchoscopy and on diagnosis of tracheobiliary fistula, patient was immediately scheduled for right thoracotomy with fistula repair so as to prevent further respiratory sequel. As these patients have poor lung compliance preoperatively they are difficult to manage intraoperatively and require proper postoperative respiratory management.
Keywords: tracheobiliary fistula, bronchoscopy, thoracotomy
Introduction
Tracheobiliary fistula is an abnormal communication between tracheobronchial tree and biliary tract. It is a rare malformation and should be included in differential diagnosis of aspiration pneumonia in infants and children. Traditionally, bronchoscopy and bronchography have been used to establish the diagnosis. This rare disorder is associated with significant (12.5%) morbidity and mortality[1].
Case Report
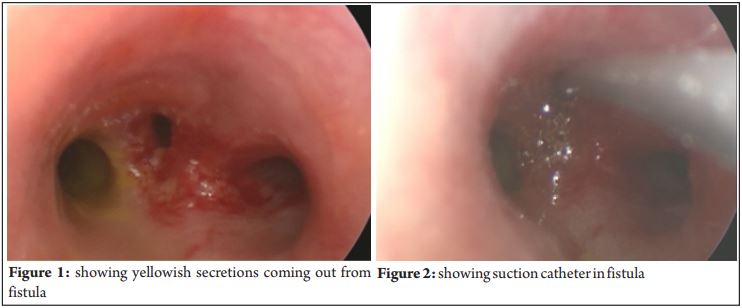
A 51 days baby was posted for bronchoscopy. He was full term cesarean section delivered baby, cried well after birth. He was admitted first on 11th day of life for aspiration pneumonia and was requiring ventilator support on and off. He was shifted to our hospital for bronchoscopy with oxygen hood on 5 l it e rs wit h SPO2 8 4 – 8 8%. On examination baby was 2.5kg, tachypnoic with respiratory rate >80, Pulse Rate 130 /m, SPO2 was 88-90%with 5 liters O2 with hood. The yellowish (bilious) secretions coming out of his mouth frequently, which need to suck out. He was passing stool of normal colour. The nasogastric tube aspiration was normal and did not show any bilious secretions. Barium swallow study was within normal limit. CT chest with contrast virtual bronchoscopy reported consolidation in right upper lobe. His Echo report revealed small VSD with Left-Right shunt. His blood investigations like complete blood count and kidney function test were within normal limits. With this patient was taken for bronchoscopy with high risk consent with post-operativeventilatorready. Premedicated with atropine 0.06mg,preoxygenated for 3 minutes with, iv ketamine 5mg given along with sevofluraneon mask. Mask ventilation was avoided so as to decrease the spoiling of remaining lung. Surgeon puts bronchoscope after relaxation with sevoflurane, anaesthesia continued through ventilating port of scope throughout the procedure, SPO2 was in between 78-90% even after ventilation. A bilious fistula was seen at carinal opening in between right and left bronchus, which was draining bile. We observed that baby’s saturation showed improvement whenever the fistula was sucked out by surgeon. Also fistula confirmation was done by guide wire placement and C-arm confirmed the tip of wire in the liver region. So it was decided to go for open thoracotomy and close the fistula immediately . Patient was intubated with ETT 3.5 on Sevoflurane without bagging with and put on ventilator, saturation improved upto 92-95%. Patient was shifted to recovery room on ventilator. After arranging blood and FFP and taking proper consent patient was scheduled for thoracotomy. He was induced with sevoflurane, fentanyl 5mg given and atracurium 2mg given, maintained with O2 and air with sevoflurane and intermittentdoses of atracurium. Right thoracotomy incision given through 6th intercostals space and with slight retraction of the lung fistula was confirmed and both ends were ligated. Intermittently we requested surgeon to release the retraction, so as to improve lung ventilation and to maintain Spo2 above 90 %. Introperatively his pulse rate remained between 120-140/minute,SPO2 remained 88-96 % . It was noticed that the right upper lobe was collapsed and was not getting inflated even after PEEP (Positive end expiratory pressure). Surgeon put intercostals drain and closure was done. Procedure was done in left lateral decubitous position and took nearly two hour. Throughout the procedure we did frequent endotracheal suctioning, even suctioning done before closure and we did not get any resistance. As soon as patient was made straight we found that it was difficult to ventilate the patient, patient started desaturating followed by bradycardia , atropine given, but no improvement was seen then considering tube mi g ht b e b l o c k ed we c hang ed t h e endotracheal tube and to our surprise it was totally blocked with blood clot. Saturation improved, heart rate improved, baby started moving again and was kept on ventilator. Next day patient was extubated and put on bubble CPAP, but O2 requirement continues for nearly 10 days , CPAP was discontinued on 10th day of operation. Ryle’s tube feed started and patient tolerated the feed very well. Patient was discharged with saturation 94-98-% without O2 and with respiratory rate nearly 40-45/min.
Discussion
Tracheobiliary fistula is a rare case, in most cases, origin of the fistula reported either from the right main bronchus (42%) or carina (42%). In only 16%, the fistula origin found to be from the left main bronchus[2]. Neuhauser et al. in 1952 reported the first case of congenital bronchobiliary fistula[3]. In our case the fistula was tracheobiliary, fistula seen at the carinal openings in between two bronchial openings. In adults it may be the result of common complication of subphrenic or liver abscesses and biliary tract obstruction[4]. However, it may be because of rare and unusual complication of traumatic thoracoabdominal wounds. Even more rare mechanism of such fistula formation is slow progressive narrowing of the common duct by the fibrosis of chronic pancreatitis, with only three cases having been reported previously[5]. Investigation of a child with a suspected bronchobiliary fistula should include bronchoscopy, bronchography and HIDA scanning. It is stated that the HIDA scan is a safe and efficient means to diagnose congenital bronchobiliar y fistula[6]. Whether the affected lobe of the liver drains normally should be confirmed, as sometimes hepatic resection of the involved lobe may be necessary in addition to resection of the fistula[7]. The embryology of this rare anomaly is still unclear. One theory is that these fistulae develop from the union of an anomalous bronchial bud with an anomalous bile duct. The fact that some fistulae are ringed by cartilage similar to bronchus gives support to this concept. The second theory is that the fistula represents a duplication of the gastrointestinal tract. Support for this theory is the fact that some fistulae found, histologically to be of esophageal origin[8]. Endoscopic closure of bronchobiliary fistula have been reported in 11 cases of which most cases were operated for hydatid cyst [8]. Our baby was posted for diagnostic bronchoscopy and had been investigated outside. Even leak test was negative. Problems associated with tracheobiliary fistula include decreased SpO2 during induction and intubation, soiling of the normal lung with infected material from the diseased lung, severe bronchospasm, hypoxemia, hypercarbia and blood loss due to extensive surgery[9,10]. For bronchoscopy, we induced our patient with sevoflurane avoiding mask ventilation so as to decrease further damage of lung and also sevoflurane has some muscle relaxant property . We were thinking of putting Fogarthy balloon in fistula so further soakage of lung can be prevented but small balloon was not available immediately. As the patient already had soiled lung, we even neither tried to do endobronchial ventilation nor to give one lung anesthesia, in fact we need to ask surgeon to release retraction in between so as to maintain SPO2 above 90%. Also repeated suctioning was required so as to prevent further soiling of an already diseaed lung till ligation of fistula. We did suctioning even before closure but after change of position we found that baby was not properly ventilated so we thought of bronchospasm, which is more common in these patients but as bradycardia follows we changed the ETT and to our surprise a huge blood clot blocks the tube. Considering persistent pneumonia and lung collapse patient was put on ventilator support and then on Bubble CPAP (Continuous positive airway pressure). The continuous positive pressure to the airway in a spontaneously breathing neonate is given so as to maintain adequate functional residual capacity within the alveoli and thus prevents atelectasis . In this method of bubble CPAP blended and humidified oxygen is delivered via short binasal prongs or a nasal mask and pressure in the circuit is maintained by immersing the distal end of the expiratory tubing in water. The depth to which the tubing is immersed underwater determines the pressure generated in the airways of the infant. As the gas flows through the system, it “bubbles” out [11] and prevents buildup of excess pressures. Some studied shows that Bubble-CPAP seems to be superior to Ventilator-CPAP in terms of treatment of respiratory distress syndrome in preterm infants due to fewer complications, shorter hospital stay, and lower cost[12]. To improve respiratory function, it is vital to continue chest physiotherapy, bronchodilators, incentive spirometry, postural drainage and antibiotics in the postoperative period. Our pediatrician weaned the baby slowly and to our efforts baby was able to maintain SPO2 upto 98% on air. He was discharged in stable conditions with good oral intake and weight gain.
Abstract
A tot a l team work is necess ar y for management of a case of tracheobiliary fistula. Preoperative, intraoperative and postoperative proper management is necessary for decreasing morbidity and mortality. Intraoperative avoidance of further spoilage of normal lung is important with postoperative ventilatory support with good analgesia, chest physiotherapy , bronchodilators, and antibiotics helps in early extubation and provides the best possible outcomes.
References
1. J James D. Fischer, MDSurgery, Canadian Journal of SurgerySurger CC , Vol 41, No 6, December 1998
2. Hyeon Yu, MD, Joseph M. Stavas, MD, and Mark Joseph, MDCongenital tracheobiliary fistula combined with hypoplastic common hepatic duct: Management by percutaneous transhepatic drainage , Radiol Case Rep.
2011; 6(4): 564.Published online 2015 Nov 6. doi: 10.2484/rcr.v6i4.564
3. Neuhauser EBD, Elkin M, Landing B. Congenital direct communication between biliary system and respiratory tract. AMA Am J Dis Child. 1952 May;83(5):654–659. [PubMed]
4. Ajay Mandal, Sanjay Sen, and Sarfaraz Jalil Baig,J minim access surg. 2008 Oct-Dec; 4(4): 111–113.
5. Bryan D. Eck , William J. Passinault, International Journal of Gastrointestinal Cancer, December 1996, Volume 20, Issue 3, pp 213–216
6. SepehrEgrari, Mohan Krishnamoorthy , Corine A. Yee, Harry Applebaum, Congenital bronchobiliary fistula: Diagnosis and postoperative surveillance with HIDA scan,Journal of pediatric surgery June 1996 Volume 31, Issue 6, Pages 785-786.
7. Gauderer MW, Oiticica C, Bishop HC. Congenital bronchobiliary fistula: management of the involved hepatic segment. J Pediatrics Surg 1993;28:452-5.
8. Yilmaz U, Sahin B, Hilmioglu F, Tezel A, Boyacioglu S, Cumhur T: Endoscopic t r e a t m e n t o f b r o n c h o b i l i a r y f i s t u l a : r e p o r t o n 11 c a s e s . Hepatogastroenterology. 1996, 43: 293-300.
9. Sukanya Mitra MD, Nidhi Bhatia MD, Nilanjan Dey MD, Usha DalalMSbBronchobiliary fistula: an anesthetic challenge! Journal of clinical anesthesia 22 August 2008
10. Agrwal A, Bose N, Gaur A, Sikora SS, Pandey CK. Bronchobiliary fistula: an anesthetic point of view.J Assoc Physicians India 2002;50: 971-3.
11. Morley, CJ; Lau, R; De Paoli, A; Davis, PG (July 2005).”Nasal continuous p o s i t i v e a i r w a y p r e s s u r e : d o e s b u b b l i n g i m p r o v e g a s exchange?”Archieves of Disease in Childhood: Fetal and Neonatal Edition. 90 (4): F343-4 doi:10.1136/adc.2004.062588. PMC 1721902.PMID 16036895.
12. Bahareh Bahman-Bijari, MD, ArashMalekiyan, MD, PedramNiknafs, MD, and Mohammad-RezaBaneshi, Bubble- CPAP vs. Ventilatory–CPAP in Preterm Infants with Respiratory Distress Iran J Pediatr. 2011 Jun; 21(2): 151–158
| How to Cite this Article: Rahate D G. Anaesthesia management of congenital tracheobiliary fistula repair. Journal of Anaesthesia and Critical Care Case Reports. May – Aug 2019; 5(2): 13-15. |
(Full Text HTML) (Download PDF)
.