Vol 8 | Issue 2 | May-August 2022 | Page: 16-18 | Swati Bharti, Ruchi Kapoor, Akanksha Rathore, Sujata Chaudhary
DOI: 10.13107/jaccr.2022.v08i02.201
Author: Swati Bharti [1], Ruchi Kapoor [1], Akanksha Rathore [1], Sujata Chaudhary [1]
[1] Department of Anaesthesiology, Critical Care and Pain Medicine, University College of Medical Sciences and Guru Teg Bahadur Hospital, Shahdara, Delhi, India.
Address of Correspondence
Dr. Swati Bharti
Department of Anaesthesiology, Critical Care and Pain Medicine, University College of Medical Sciences and Guru Teg Bahadur Hospital, Shahdara, Delhi, India.
E-mail: swatibharti2012@gmail.com
Abstract
Introduction: Presence of an intraoral swelling may pose difficulty in laryngoscopy, glottic visualisation and endotracheal intubation using the conventional Mcintosh laryngoscopy. Not only does the mass anatomically hampers the laryngoscopy but also there is risk of trauma to the mass which may bleed and create further difficulty in securing the airway.
Case presentation: An 18-year-old boy presented to us for excision of a mass arising from hard palate since 1½ years. CECT PNS was suggestive of large well-defined lytic expansile area seen in upper alveolus and adjacent hard palate extending into the anterior part of nasal cavity abutting bilateral inferior turbinate and obliterating anterior part of nasal cavity thus a contraindication for nasal intubation. On airway examination, mouth opening was adequate with MPC 1, loose upper incisors, 3×3 cm swelling on hard palate and decreased nasal patency. As the surgeon had to operate in the midline, therefore a plan for retromolar intubation was made to secure the airway using paraglossal approach for direct laryngoscopy with a Millers blade keeping in mind that endotracheal tube shouldn’t interfere in the operative field.
Conclusion: Retromolar intubation can be used successfully for securing airway for surgical procedures in oral cavity when nasotracheal intubation is not possible, and surgical access to airway is best avoided.
Keywords: Retromolar tracheal intubation, Midline hard palate cyst, Airway management
Introduction
Direct laryngoscopy and endotracheal intubation under vision continues to be the gold standard for airway management. Though conventional laryngoscopy is done with Mcintosh blade, however, it has its own drawbacks like its curvature obliterates line of view especially in subjects where space in mouth is limited. Also, it may not be feasible to displace the entire tongue leftwards as mandated by this technique of intubation. Retromolar technique of endotracheal intubation with paraglossal approach using Millers blade can prove to be a useful alternative for securing airway in such scenario without requiring any special equipment [1].Intraoral swelling pose a unique challenge to anaesthesiologist wherein presence of the swelling makes the laryngoscopy and glottic visualization difficult leading to difficulty in endotracheal intubation and thus anticipating difficult airway. The retromolar intubation comes to rescue as it prevents any trauma to the mass as compared to the midline oral intubation using Mcintosh laryngoscope. In this technique laryngoscope blade is inserted from the extreme corner of the mouth so that it passes immediately beside the tongue and then next to the tonsillar pillar on the right side of the oropharynx and upon visualization of the glottic aperture, endotracheal tube (ETT) is inserted from the lateral aspect of the mouth passing through the retromolar space [2].We present a unique case of intraoral median hard palate swelling where nasotracheal route of intubation was not possible and conventional laryngoscopy could have caused trauma to the mass thus retromolar approach for tracheal intubation was used to secure the airway precluding surgical airway.
Case Report
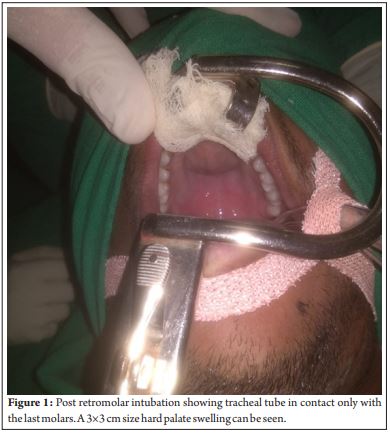
An 18-year-old male with hard palate swelling since 1½ years presented for excision of the mass under general anaesthesia. The patient was informed that data from the case would be submitted for publication and gave his consent. The swelling was insidious in onset, progressive in nature, no aggravating or relieving factor and was associated with mild on and off pain radiating to the central incisors. There was no history of dysphagia, weight loss, loss of appetite, intraoral discharge, ear discharge or earache. No significant past history and family history. Airway assessment revealed adequate mouth opening (MPC 1) and normal neck range of motion and loose upper incisors. A 3×3 cm size firm, non-tender, non-fluctuant, midline hard palate swelling seen with normal overlying mucosa. Bilateral nasal spur was present abutting the nasal cavity. Thus, nasotracheal intubation by fibreoptic bronchoscope was ruled out. CECT PNS was suggestive of large well-defined lytic expansile area seen in upper alveolus and adjacent hard palate extending into the anterior part of nasal cavity abutting bilateral inferior turbinate and obliterating anterior part of nasal cavity suggestive of bone cyst/dental cyst. FNAC confirmed no evidence of cancer. Patient was accepted for anaesthesia under ASA I category. Difficult airway cart was kept ready. In the operating room, standard monitors were attached and a 20G intravenous (IV) catheter was secured. Preoxygenation was done with 100% oxygen. General anaesthesia was induced with injection morphine 6 mg IV and injection propofol 100 mg IV with 50% oxygen in nitrous oxide and isoflurane (1%). After ensuring effective ventilation, injection vecuronium 6 mg IV was given. After three minutes of bag and mask ventilation, direct laryngoscopy was performed with a size 3 Miller’s blade using paraglossal approach. Airway was secured with 8.0 mm internal diameter endotracheal tube (ETT) placed behind the last molar tooth on the left side in the retromolar space so that ETT doesn’t interfere in the operative field as demanded by the surgeon. After intubation, throat pack was inserted. (Fig. 1)Anaesthesia was maintained with 33% O in N O and Isoflurane 2 2(1-0.8%) to achieve a MAC of 1-1.2. Adequate muscle relaxation was maintained with intermittent doses of injection vecuronium 1 mg IV. All vital parameters were stable in the intra-operative period. At the end of the surgery neuromuscular blockade was reversed with injection neostigmine 3.5 mg IV and injection glycopyrrolate 0.6 mg IV. After recovery of neuromuscular blockade, regular respiration and good reflexes, patient was extubated and shifted to post anesthesia care unit (PACU). Humidified oxygen was given by face mask and vital monitoring was done in PACU. Post anaesthesia course was uneventful.
Discussion
Retromolar space is a hidden space located between the last molar and the ascending ramus of the mandible. It is bounded anteriorly by the last erupted molar, posteriorly by the ramus of the mandible, superiorly by the maxillary tuberosity, and inferiorly by the retromolar trigone. Retromolar space dimensions measured using dental pentomograms reveal that the space is large enough to accommodate 8.0 mm endotracheal tube with outer diameter of 10.8 mm without kinking [3]. Adequacy of this space can be confirmed by placing finger behind the distal molar [4].Retromolar intubation prevents obliteration of surgical field in case of midline oral surgeries as in this case. Paraglossal approach prevents trauma from direct impingement of fragile palatal lesion as blade is introduced lateral to tongue. In the present case nasal intubation could not be done due to the presence of bilateral nasal spur.Paraglossal approach for retromolar intubation using Millers blade is safer than the conventional midline approach especially in the presence of a midline hard palate swelling as it will never interfere with the swelling in the midline as the laryngoscope blade is introduced from one side of the tongue laterally and the ETT is inserted from the angle of the mouth, reducing the chances of trauma or injury to the swelling. Millers blade has a shallow base and a narrower tip. The tongue is straight with a slight upward curve near the tip. In the cross section, the flange, web and tongue form a C with the top flattened. Bulb is placed distally close to the tip for better visualisation. It has been seen that the narrow based straight blade occupy less space than the conventional curved blade, thus, causing less disturbance to the internal oral structures while manoeuvring the scope inside [5]. Since, it was a case of an anticipated difficult airway, so we kept the difficult airway cart ready in the OT before induction of anaesthesia. Our plan A was to intubate the trachea by retromolar technique using paraglossal approach with Millers straight blade. However, videolaryngoscope (VL) was kept ready if plan A failed. We were reluctant to use VL in the first attempt as the swelling was in the midline and VLs are inserted from the midline which could have caused injury to the cyst while adjusting the scope inside the oral cavity. Fibreoptic oral intubation under general anaesthesia or any other technique of intubation through midline could have caused trauma to the mass, further, leading to the risk of aspiration. So, the next step would have been either submental intubation or tracheostomy, both being invasive techniques having their own risks and complications. Using retromolar technique of intubation we could easily secure the airway avoiding the invasive surgical route and at the same time, it provided an unobstructed operative field to the surgeon.As surgeon demanded the ETT to be placed in the retromolar trigone for better visualisation of the field, 8.0 mm internal diameter polyvinyl chloride ETT was used for securing the airway using retromolar technique where the ETT was placed behind the last molar tooth on the left side. South Polar Ring-Adair-Elwin tube could have also been used in the present scenario. But it comes with its own drawbacks. Firstly, the preformed bend makes suctioning difficult through them and offers more resistance than same sized conventional tubes. Secondly, risk of inadvertent extubation while the surgeon is removing or adjusting the gag or tube compression, if the gag has no slit. Thirdly, these tubes are designed to fit the average patient, a tube may be either too long or too short for a given patient. These conditions can be easily averted by using conventional ETT with retromolar technique of tracheal intubation. Aggarwal et al reported successful intubations using paraglossal straight blade technique in anticipated difficult airways having Mallampati class 3 and 4 [6]. Jindal et al reported easier glottic visualization and intubation with Millers blade using paraglossal approach as compared to traditional approach using Mcintosh blade [2]. It allows adequate dental occlusion, therefore, helps in intraoperative intermaxillary fixation in patients with pan facial trauma [7]. This technique can also prove to be useful in paediatric anticipated difficult airway scenarios where awake fibreoptic intubation is next to impossible owing to the lack of cooperation from patient side.It is a non-invasive, non-traumatic, time efficient and easy to perform method of securing the airway without requirement of any special device. Tube patency can be easily monitored [8]. However, limited space may be encountered due to impacted or erupting third molar in some patients. Injury to adjacent buccal mucosa, long buccal nerve palsy is another possible disadvantage.This technique prevents the risks and complications associated with invasive procedures like submental intubation or tracheostomy. Thus, retromolar approach for tracheal intubation provides an alternative technique to secure the airway when conventional oral or nasal routes for tracheal intubation are either not available or unsuitable. It is therefore advocated that anesthetists should gain expertise of intubation using straight blade also as there may be instances such as above where Mcintosh blade is best avoided.
Conclusion
We conclude that retromolar intubation can be used successfully for securing airway for surgical procedures in oral cavity when nasotracheal intubation is not possible, and surgical access to airway is best avoided. This time-tested technique of tracheal intubation is simple and reliable but should be practiced routinely so that it can be used effectively in cases of emergency.
Clinical message
Intraoral swelling makes laryngoscopy, glottic visualisation and endotracheal intubation difficult especially when using the conventional Mcintosh laryngoscopy. Not only does the mass anatomically hampers the laryngoscopy but also there is risk of trauma to the mass which may bleed and create further difficulty in securing the airway. Thus, raising the need for an alternative method of securing the airway in such scenarios. Retromolar tracheal intubation is an alternative method of securing airway in patients where orotracheal or nasotracheal intubation may be difficult or unsuitable. This technique avoids surgical access to airway
References
1. Swain BP, Nag DS, Samaddar DP, Swain A, Srividhya, Panigrahi B, et al. Does miller straight blade and paraglossal technique provide better laryngoscopy than traditional macintosh blade standard technique – A comparative study? Middle East Journal of Anesthesiology. 2017;24(2):111-8.
2. Jindal P, Khurana G, Gupta D, Chander U. Can Paraglossal Approach be an Effective Alternative to the Conventional Laryngoscopy in Routine Anesthesia Practice- A Comparative Study. J Anesth Clin Res. 2014, 5 :406. doi:10.4172/2155-6148.1000406.
3. Nguyen LT, Thakar SD, Truong AT, Truong DT. Orotracheal Intubation Using the Retromolar Space: A Reliable Alternative Intubation Approach to Prevent Dental Injury. Case Rep Anesthesiol. 2016;2016:3529415.
4. Lee SS, Huang SH, Wu SH, Sun IF, Chu KS, Lai CS, et al. A review of intraoperative airway management for midface facial bone fracture patients. Ann Plast Surg. 2009;63(2):162-6.
5. Dorsch JA, Dorsch SE. Laryngoscopes. In: Dorsch JA, Dorsch SE (Eds). Understanding Anesthesia Equipment, 5th Edition. Philadelphia: Lippincott Williams and Wilkins; 2007.
6. Agrawal S, Asthana V, Meher R, Singh DK. Paraglossal Straight Blade Intubation Technique- an Old Technique Revisited in Difficult Intubations: A Series of 5 Cases. Indian J. Anaesth. 2008;52(3):317-20.
7. Malhotra N. Retromolar intubation: a technical note. Indian J. Anaesth. 2005;49(6):467-8.
8. Dutta A, Kumar V, Saha SS, Sood J, Khazanchi RK. Retromolar tracheal tube positioning for patients undergoing faciomaxillary surgery. Can J Anaesth. 2005;52(3):341.
| How to Cite this Article: Bharti S, Kapoor R, Rathore A, Chaudhary S | Retromolar Approach for Tracheal Intubation: Rescue Technique in a Rare Case of Hard Palate Cyst- A Case Report | Journal of Anaesthesia and Critical Care Case Reports | May-August 2022; 8(2): 16-18. |