Vol 9 | Issue 1 | January-April 2023 | Page: 04-08 | Chetan Mehra, Charu Shrotriya, Chitra Chatterji
DOI: https://doi.org/10.13107/jaccr.2023.v09i01.211
Author: Chetan Mehra [1], Charu Shrotriya [1], Chitra Chatterji [1]
[1] Department of Anaesthesiology, Critical Care and Pain, Indraprastha Apollo Hospital, New Delhi, India.
Address of Correspondence
Dr. Chetan Mehra,
Consultant Anaesthesiologist, Department of Anaesthesiology, Critical Care and Pain, Indraprastha Apollo Hospital, New Delhi, India.
E-mail: Chetanmehra@yahoo.co.in
Abstract
Our case illustrates the management of a life-threatening difficult airway scenario, in a young male with an in-situ metallic tracheal stent, who was scheduled for excision of the granulation tissue compromising the lumen of stent. He presented with occasional difficulty in breathing, without stridor. An out-patient based nasal video laryngoscopy performed a week prior revealed, granulations at the proximal end of the stent.
Inhalation induction with preservation of spontaneous respiration was performed. Eventually, the patient landed with inability to ventilate and intubate, necessitating a need for emergency establishment of a definitive airway. The presence of metal stent prevented establishment of percutaneous cricothyroidotomy or tracheostomy (FONA- front of neck access).
A paediatric rigid bronchoscope shoved through the granulation tissue, finally established oxygenation. It was used as a conduit for passage of a fogarty catheter, over which a smaller sized endotracheal tube was finally railroaded.
Surgical excision of granulation tissue was performed over endotracheal tube using micro-scissors and patient finally extubated.
This case scenario highlights the importance of a cautious approach towards a potential catastrophe presented by partial obstructed tracheal stent. This requires an effective communication between surgical and anaesthesia teams, as in most cases, an access to airway is limited for anaesthesiologists.
Keywords: Tracheal stent, Rigid bronchoscope, Fogarty catheter
Introduction
Tracheal stenting is performed to channelize a stenosed tracheal segment in situations where a surgical reconstruction is not feasible for various reasons [1]. Such conditions include tracheal stenosis caused by benign or malignant tracheal lesions and traumatic neck injuries involving tracheobronchial tree. There has been a gradual increase in use of tracheal stents with an advancement in palliative care for this category of patients [1]. Over a long term, the patients with tracheal stents may present to health care facilities with issues related to complications of stents. These include mucus hyper-secretions, lower respiratory tract infections, hemoptysis, granuloma formation or stent migration [2, 3]. Granulation has been reported in 0-20% of cases and migration and deviation reported in 10-22% of cases in which silicon stents were used.Tracheal stents can be bare metallic, silicone or hybrid, by virtue of their material. Hybrid stents combine the properties of both conventional silicone stents and metal stents. They prevent major complications, including granulation, tumor invasion and breakage of the metal part, as are reported with metal stents. Silicone stents prevent tumor invasion [4]. Bare metallic stents possess a higher risk of granuloma formation [5, 6]. This subset of patients pose an additional airway challenge when they need a surgical procedure for their airway related issues and require an effective communication between surgical and anaesthesia teams. Here, we present a case of a young patient with metallic tracheal stent, who presented to our hospital with difficulty in breathing. He was scheduled to undergo laser excision of granulation tissues partially obstructing proximal orifice of the stent.
Case Presentation
A 20 year old, 70 kg male patient presented to hospital with complaints of difficulty in breathing without associated stridor. He had suffered a road traffic accident five years prior, following which he underwent laryngotracheal reconstruction and a tracheostomy tube was placed. He developed tracheal stenosis after tracheal decannulation. Tracheal stenosis was addressed with balloon tracheal dilatation, which was unsuccessful and later a bare metal stent was inserted. The details of tracheal stent (with regard to its length, distance of proximal orifice from vocal cords and distance of distal orifice from carina) and anaesthesia for the same were not available. Patient had been evaluated on an outpatient basis a week prior, as a part of routine follow up, by an otolaryngologist at our center. Flexible video laryngoscopy revealed granulations at the proximal end of the stent. At this point in time, he was asymptomatic.
Pre-operative Evaluation
On the day of admission, patient presented with occasional difficulty in breathing, without associated symptoms of respiratory distress. His hemodynamic parameters were normal and he had oxygen saturation of 100% on room air. Patient was scheduled for laser excision of granulation tissue from the proximal orifice of metal stent. His medical history was unremarkable. He was well built, physically active and carried out his routine daily activities without much discomfort. Upper airway examination was normal, apart from the fact that he could not complete one sentence at one stretch. He had to take a break for a breath in between while completing a single sentence. He did not have any preferred position which would exacerbate or relieve his symptoms, nor did he have any history of recurrent upper airway infections or increase in pulmonary secretions. An important input by surgical team suggested that patient’s laryngeal inlet (i.e. tracheal stent orifice size) would allow 5.0 mm ID (internal diameter) laser ETT (endotracheal tube), as estimated roughly by pre-operative flexible video laryngoscopy [7]. Blood investigations were within normal limits. Patient was taken up for surgery with ASA 2 (American Society of Anesthesiology) physical status by virtue of prior laryngotracheal interventions and a possibility of difficult airway scenario. An extra help of a senior anaesthesia colleague was sought while inducing this patient for surgery.Consent was taken for anaesthesia and surgery, explaining the concerns of difficulty in accessing the airway and possibility of stent dislodgement.
Intraoperative Management
Plan of anaesthesia:
Plan of anaesthesia was induction with sevoflurane and preservation of spontaneous respiration, followed by laryngoscopy and assessment of the vocal cords and proximal stent orifice. This would be followed by the insertion of a laser MLS (micro-laryngoscopy) ETT for assisting laser excision of granulation mass.The goal of anaesthesia was to maintain a patent airway, allow a safe surgical exposure, and have the patient fully awake and cooperative, with preserved airway reflexes, at the end of surgery.Preparation for possible difficult airway scenario: Anaesthesia workstation was checked for oxygen delivery and oxygen failure measures. MacIntosh, video laryngoscope and flexi-tip McCoy laryngoscope of sizes 3 and 4, supraglottic airway devices (Laryngeal Mask Airways – including Proseal and Intubating LMA of sizes 3, 4 and 5), jet ventilator, airway bougie (adult and paediatric) and airway exchange catheter, fiberoptic bronchoscope, adult sized rigid bronchoscope and a cricothyroidotomy set were kept standby. There was a limited scope, if any, for FONA (front of neck access), because of presence of a metal tracheal stent, making it challenging for cricothyroidotomy or tracheostomy [1].
Conduct of anaesthesia:
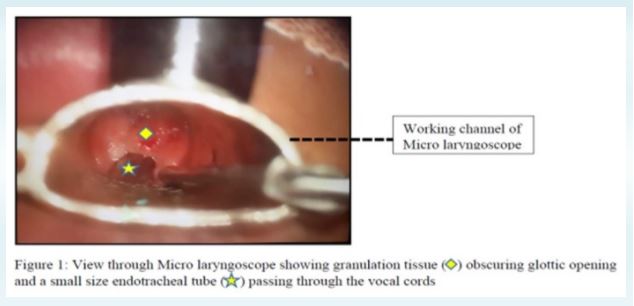
Patient was transferred to operating theater after confirmation of fasting status. Routine monitors were connected and a wide bore intravenous access secured. Patient was oxygenated with 100% oxygen till the end tidal oxygen concentration reached 90% in supine position. Inj glycopyrrolate 0.2mg was administered to decrease airway secretions.Inhalation anaesthesia was initiated with careful titration of sevoflurane in 100% oxygen. With progressive deepening of plane of anaesthesia, an obstructive pattern of breathing was observed. Patient was able to maintain oxygen saturation till this time as his spontaneous respiration was still preserved. His breathing was assisted with application of CPAP (Continuous Positive Airway Pressure >30 cm water). Although there was a disappearance of EtCO (end-tidal carbon dioxide) trace on 2monitor, a complementary movement of rebreathing bag with patient’s respiration was quite reassuring, which indicated a patent airway.In an attempt to release upper airway obstruction, a nasal airway was nd inserted, which obviously was not a solution for the same. A 2generation supraglottic airway device (Proseal # 4) was inserted, in the same plane of anaesthesia. Unluckily, patient was not able to be ventilated with the same and an obstructive pattern of ventilation continued. Call for help was initiated. A direct laryngoscopy with flexi-tip McCoy blade # 4 was attempted, which revealed Cormack Lehane grade I laryngeal inlet, with clearly visualized vocal cords, that seemed to be edematous. Laryngeal inlet was completely obscured by mucosal proliferation (Figure 1). It was decided to wake up the patient if possible and reschedule the surgery or a later date. But worsening hypercapnia caused by ineffective gas exchange would not allow patient to be woken up [8].An unsuccessful attempt was made to negotiate 5.0 mm ID laser ETT through the laryngeal inlet. Progressively smaller sized endotracheal tubes aided with paediatric bougie were unsuccessfully tried. Subsequently, ventilation through LMA was also not possible.In the further course of next few minutes, patient started desaturating and soon developed atrial fibrillation, followed by hemodynamically unstable ventri cular tachyc ardia , whi ch wa s managed pharmacologically and electrically to finally revert to sinus rhythm. An arterial cannula was secured. Arterial blood gas analysis (ABG) showed severe respiratory acidosis, with preserved oxygenation (pH 6.9, PaCO 110). 2 Cardiothoracic surgical team was immediately alerted for set up of peripheral cardio-pulmonary bypass (CPB) to establish oxygenation.
Concerns to address at this point were:
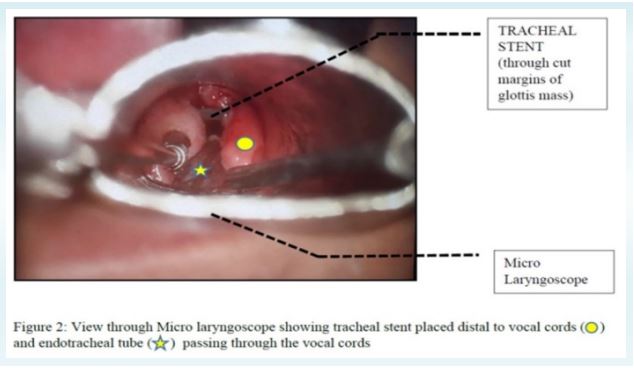
Front of neck access was not feasible option with tracheal stent in situ, with high chances of stent damage or migration1Meanwhile a paediatric rigid bronchoscope (size 3 mm ID, 5 mm outer diameter) was quickly arranged and was forcibly pushed through the glottic opening and through the granulation mass, keeping in my mind that this maneuver could lead to dislodgement of growth and cause bronchial obstruction. A give away feeling was felt with the passage of bronchoscope beyond the mass. Following this, ventilation could be achieved, which came as a tremendous relief at that moment.Anaesthesia was now maintained with TIVA (Total Intravenous Anaesthesia) using propofol, while assisting respiration via the side arm of the ventilating bronchoscope. A Fogarty Embolectomy Catheter (Edwards Lifesciences; size 3 Fr; 1mm ID; 80 cm length) was then inserted through the working channel of bronchoscope. A smaller sized ETT with 4 mm ID was railroaded over the Fogarty catheter, after removal of bronchoscope, in order to maintain oxygenation (Figure 2) [3, 4]. Surgical plan was finally changed from laser excision to knife assisted excision of the mucosal growth around the endotracheal tube. Once the patency of the airway was established with EtCO and 2bilateral equal air entry in lungs (ruling out the possibility of an iatrogenic pneumothorax), the plane of anesthesia was deepened using propofol and relaxation achieved by atracurium. Surgical (partial) excision of the granulation tissue was done around the ETT using scissor micro-forceps (without the use of laser). After excision of tissue, a clear view of stent could be seen through edematous vocal cords. We contemplated a need to extract the stent in the same sitting, but this plan was deferred. This decision was based upon the fact that over a period of time the metal stent gets incorporated into the airway wall and its mesh becomes covered with mucosa [9].
Post-op management, monitoring and recovery
At the end of the procedure, it was decided to give a trial of extubation. By this time, patient achieved stable hemodynamics with normal parameters in ABG analysis. Neuromuscular blockade was reversed with neostigmine 0.05 mg/kg and glycopyrrolate 0.01 mg/kg and clinically assessed for the return of neuromuscular function [10]. After confirmation of a negative cuff leak test [11] and acceptable extubation criteria, reversible extubation [12] was performed by reinserting the Fogarty catheter through the endotracheal tube and extubating trachea over the Fogarty catheter in a ramped up position [13]. He was nebulized with salbutamol and budesonide, followed by oxygenation with facemask @ 4 l/min. He was observed for any signs of respiratory distress in the OR for about 45 minutes post extubation. Fogarty catheter was then removed.Patient was then shifted to ICU for further observation. Patient was completely oriented to time, place and person and showed no signs of hypoxic brain injury the following day
Discussion
Patients with a tracheal stent may present with granulation tissue growth within the stent lumen, causing partial airway obstruction. The metal edge of the stent exerts circumferential pressure on the tissue and is likely to cause airway inflammation and subsequent granulation tissue formation [3]. A pre-operative airway assessment may not definitely correlate with ease of ventilation or intubation in such cases. A more appropriate assessment can be achieved by awake fiberoptic laryngoscopy just before proceeding with anaesthesia induction in such a patient. Direct laryngoscopy may reveal clear visualization of the glottic opening but introduction of ETT may be difficult, as in our case. An immediate preoperative period bronchoscopy or CT scan will also help to assess the extent of the laryngotracheal compromise, distance of the stent from the glottis and the extent of the granulation [15].This presents with a challenging and potential difficult airway scenario, especially since the scope for FONA is limited [1]. Maintenance of spontaneous respiration until such a time that oxygenation and ventilation is established remains key for patient survival. To establish a tracheostomy in patients with tracheal stents is challenging and may lead to stent damage, compression or misplacement and airway compromise [5]. It has been suggested that it is essential to maintain a width of at least 1 cm between the proximal edge of the stent and the vocal folds to prevent discomfort and obstructive complications, such as laryngeal edema, stent migration and granulation tissue [14]. In our case, this distance could not be assessed on direct visualization or through video laryngoscopy. A pre-formulated plan with awake fiberoptic evaluation and intubation is the safest technique [16, 17], although one needs to have alternate plan B and C charted out. Good communication as well as coordination between the teams involved are the key components to design a successful anesthetic plan.The four basic ventilation methods that can be used for patient requiring anaesthesia for tracheo-bronchial procedures are [18]:
a. Spontaneous ventilation with inhalational anaesthesia along with topical anaesthesia.
b. Apneic oxygenation with or without oxygen insufflation.
c. Intermittent positive pressure ventilation with bronchoscopic ventilation.
d. Jet ventilation during TIVA.
Currently, there are no formal consensus amongst difficult airway societies regarding the best method to approach a difficult airway with a tracheal stent in situ [1].However, Lawrence et al, have proposed an airway algorithm considering awake ECMO or awake fiberoptic intubation until a definitive airway is secured [19]. VV-ECMO (Veno-venous Extracorporeal Membrane Oxygenation) use has been described for extraction of a hybrid tracheal stent [3]. CPB and ECMO, both of which can be a life-saving in near or total occlusion of the airway, have been used for tracheal surgery [20, 21].Recently, high flow nasal oxygenation device (HFNO) has been extensively used for upper airway surgeries. It can provide oxygen both to patients who can breathe spontaneously and to those who are apneic; further, this technique does not interfere with bag-mask ventilation, attempts at laryngoscopy for tracheal intubation, and surgical procedures conducted in the airway [22].
Limitations
• Sevoflurane was chosen to facilitate the adjustment of anaesthesia depth in this case. However, because adequate ventilation is a prerequisite for emergence from anaesthesia with sevoflurane, anaesthesia management with TIVA, which does not depend on ventilation, may be more appropriate.
• Details of tracheal stent were not known (with respect to its size, length, etc)
• A pre-induction flexible bronchoscopy performed in the OR (rather than completely relying on surgeon’s input) would have helped us to modify our plan of anaesthesia. Stenosis quantification by CT or bronchoscopy have comparable results [7].
• CPB and/or ECMO were not kept as a standby in our anaesthesia plan.
Conclusion
This case scenario highlights the importance of a cautious approach towards a potential catastrophe presented by partial obstructed tracheal stent. An appropriate assessment of patency of stent can be achieved by a preoperative awake fiberoptic laryngoscopy or nasal endoscopy. This requires an effective communication between surgical and anaesthesia teams, as in most cases, an access to airway is limited for anaesthesiologists. A coordinated team effort involving otolaryngologists, radiologist, anaesthesiologist and occasionally cardiothoracic personal is needed for a successful management of such case, as described.
References
1. Navas-Blanco, Jose R et al. “Emergent airway management in a patient with in situ tracheal stent: A lesson learned.” Saudi journal of anaesthesia vol. 12,4 (2018): 626-628.
2. Sriram, K., Robinson, P. Recurrent airway obstructions in a patient with benign tracheal stenosis and a silicone airway stent: a case report. Cases Journal 1, 226 (2008).
3. Rampey AM, Silvestri GA, Gillespie MB. Combined endoscopic and open approach to the removal of expandable metallic tracheal stents. Arch Otolaryngol Head Neck Surg. 2007;133:37-41.
4. Sanchit A, Barak C, Jochen H, Pierre D, Kurt R. Practical anesthetic considerations in patients undergoing tracheobronchial surgeries: a clinical review of current literature. Journal of Thoracic Disease 2016;8(11):3431-3441.
5. Davis N, Madden BP, Sheth A, Crerar-Gilbert AJ. Airway management of patients with tracheobronchial stents. Br J Anaesth. 2006 Jan;96(1):132-5.
6. Zakaluzny S. Complications of tracheobronchial airway stents. Otolaryngol Head Neck Surg. 2003;128(4):478–88.
7. Morshed K, Trojanowska A, Szymański M, et al. Evaluation of tracheal stenosis: comparison between computed tomography virtual tracheobronchoscopy with multiplanar reformatting, flexible tracheofiberoscopy and intra-operative findings. Eur Arch Otorhinolaryngol 2011;268:591-7.
8. Cheng Q, Zhang J, Wang H, Zhang R, Yue Y, Li L. Effect of acute hypercapnia on outcomes and predictive risk factors for complications among patients receiving bronchoscopic interventions under general anesthesia. PLoS One. 2015;10:e0130771.
9. Burningham AR, Wax MK, Andersen PE, et al. Metallic tracheal stents: complications associated with long-term use in the upper airway. Ann Otol Rhinol Laryngol 2002; 111:285–290.
10. Manfred B, Jennifer M, Claude M, Eva K, Heidrun L, Kurt U. use of a train-of-four ratio of 0.95 versus 0.9 for tracheal extubation: an exploratory analysis of POPULAR data. British Journal of Anaesthesia. Volume 124, Issue1, P63-72, January 01,2020.
11. Daniel DB. The cuff-leak test: what are we measuring? Critical Care. 2005; 9(1):31-33.
12. Benumof and Hagberg’s Airway Management. 2013: 1018-1046.e7.
13. Sato, S., Chaki, T., Onaka, T, et al. anesthetic management of tracheal stent extraction using a double gum elastic bougie technique. JA Clin Rep 8,9 (2022).
14. Bourinet V, Raguin T, Fortin M, et al. experience with transcordal silicone stents in adult laryngotracheal stenosis: a bicentric retrospective study. Respiration. 2018;95:441-8.
15. Daniel N, Tim S, Piotr K. Airway stents: anaesthetic implications, Continuing Education in Anaesthesia Critical Care & Pain, Volume 10, Issue 2, April 2010, Pages 53–58.
16. Iseli TA, Iseli CE, Golden JB, Jones VL, Boudreaux AM, Boyce JR, et al. Outcomes of intubation in difficult airways due to head and neck pathology. Ear Nose Throat J. 2012;91(3):E1-5.
17. Collins SR, Blank RS. Fiberoptic intubation: an overview and update. Respir Care. 2014;59(6):865–78; discussion 878-80.
18. Pathak V, Welsby I, Mahmood K, et al. Ventilation and anesthetic approaches for rigid bronchoscopy. Ann Am Thorac Soc 2014;11:628-34.
19. Weinberg L, Graham J, Meyerov J, Moshinsky JA, Aitken SAA, Spanger M, Knight S. Tracheal Stent Buckling and In-stent Stenosis: A Proposed Airway Management Algorithm for Airway Obstruction for Patients With Tracheal Stents. J Cardiothorac Vasc Anesth. 2022 Aug;36(8 Pt B):3139-3146.
20. Soeda, R., Taniguchi, F., Sawada, M., Hamaoka, S., Shibasaki, M., Nakajima, Y., Hashimoto, S., Sawa, T., & Nakayama, Y. (2016). Management of Anesthesia under Extracorporeal Cardiopulmonary Support in an Infant with Severe Subglottic Stenosis. Case reports in anesthesiology, 2016, 6871565.
21. Gao H, Zhu B, Yi J, Ye TH, Huang YG. Urgent tracheal resection and reconstruction assisted by temporary cardiopulmonary bypass: a case report. Chin Med Sci J. 2013 Mar;28(1):55-7.
22. Kim HJ, Asai T. High-flow nasal oxygenation for anesthetic management. Korean J Anesthesiol. 2019;72(6):527-547.
| How to Cite this Article: Mehra C, Shrotriya C, Chatterji C Paediatric Rigid | Bronchoscope and Fogarty Embolectomy Catheter as a Rescue in Successful Management of a Patient with Metallic Tracheal Stent In-Situ: A Case Report | Journal of Anaesthesia and Critical Care Case Reports | January-April 2023; 9(1): 04-08 | https://doi.org/10.13107/jaccr.2023.v09i01.211 |